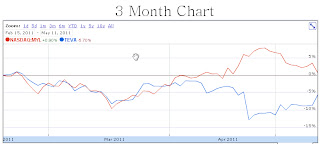
Ariad Pharmaceuticals, Inc. (NASDAQ: ARIA) is a cancer-focused biotechnology located in Cambridge, Massachusetts. The company is discovers and develops drugs aimed at treating human diseases at the cellular level. The main product candidates are ridaforolimus, ponatinib, and AP26113. In 2007, Ariad reached a collaboration agreement with Merck for the development of ridaforolimus. Under the agreement, Ariad received an upfront payment of $75 million and has received $53.5 million in milestone payment for the initiation of Phase 2 and 3 trials. The development, manufacturing, and commercialization costs are evenly split between the companies.1
Ponatinib (AP24534) and Tyrosine Kinase Inhibitors
Ponatinib is a novel, orally active tyrosine kinase inhibitor (TKI). The molecule is active against a range of tyrosine kinases including all forms of BCR-ABL (therefore called a pan-BCR-ABL inhibitor). BCR-ABL is prevalent in chronic myelogenous leukemia (CML) and Philadelphia chromosome positive (Ph+) acute lymphoblastic leukemia (ALL). The are dozens of mutated forms of BCR-ABL and mutation is one of the resistance mechanisms employed by cancer cells. Ponatinib may also inhibit Flt3 (AML), and FGFR and VEGFR in solid tumors.
An important saying in oncology is that whatever the body does normally, it can do abnormally. Since cancer cells are normal cells gone awry, they share many of the same molecular mechanisms. Tyrosine kinases are vital parts of normal cellular functioning. However mutated forms may give rise to cancerous cells. Although at first glance it may seem ideal that TKIs target a wide range of kinases, they may also interfere with the functioning of normal cells and there exists a potential for secondary malignancies. Combined with the fact that Gleevec has helped convert CML into a chronic disease, long-term monitoring is of great importance.
BCR-ABL fusion gene allows for escape from growth regulation à activated as functional oncogene à increased kinase activity à cell proliferation, inhibition of apoptosis, and malignant clones.
Imatinib (Gleevec) was the first TKI active against BCR-ABL. Despite wonderful activity, patients' tumors develop resistance to Gleevec. This ushered in the another generation of TKIs targeting BCR-ABL, dasatinib (Sprycel, Bristol-Myers Squibb; NYSE: BMY)2 and nilotinib (Tasigna, Novartis; NYSE: NVS)3, which both are active against BCR-ABL. Both drugs are approved for patients whose cancers no longer respond to and are intolerant to Gleevec. Sprycel and Tasigna have warning of arrhythmia known as QT interval prolongation. This concern is addressed for all new drugs and will be closely monitored for ponatinib since molecules in the same class have been shown to cause QT prolongation.
ENESTnd Study- Nilotinib showed superior results compared to imatinib in terms of CCyR and MMR at 12 months for newly diagnosed patients 4
DASISION Study- Dasatinib showed superior results compared to imatinib in terms of CCyR and MMR at 12 months for newly diagnosed patients 5
There are over 40 identified mutations in Gleevec binding site in CML patients. The T315I mutations confers resistance to Gleevec, Sprycel, and Tasigna. The emergence of this mutation requires change of therapy to interferon alpha or stem cell transplant. This unmet clinical need is addressed by ponatinib since it is claimed as a pan-BCR-ABL TKI.
Other TKIs include Erlotinib (Tarceva), Lapatinib (Tykerb), gefitinib (Iressa), sunitinib (Sutent), and sorafenib (Nexavar). These agents are approved for a variety of cancers such as non-small cell lung cancer, renal cell carcinoma, and breast cancer.
Background on Leukemias (ALL and CML)
- Leukemias are malignancies of hematopoietic cells in the bone marrow and blood
- They occur in either the myeloid lineage (basophils, eosinophils, neutrophils, monocytes, platelets, erythrocytes) or lymphoid lineage (T lymphocytes and B lymphocytes)
- Type of leukemia reflect maturity of hematopoietic stem cells from which it developed
- Acute Leukemias- early cells in the myeloid (AML) or lymphoid (ALL) lineage
- Chronic Leukemias- genetic abnormalities occur in later stages of white blood cell development
- Acute Lymboblastic Leukemia
- Incidence: 5,760 in 2009
- Deaths: 1,400 in 2009
- Patients typically attain remission, but it is difficult to keep them in remission
- Poor prognostic factors: L2 or L3 (based on French American British System, 70% of adult ALL); Ph+ (30% of adult ALL); abnormal cytogenetics; Age > 30; white blood cell >30K; platelet count < 10K; delayed remission; male > female; African american; CNS disease; enlarged liver or spleen; mediastinal mass.
- Goal: Achieve complete remission and continue therapy. CR achieved in 65-85%; relapse is common. Gleevec is added to the regimen if cancer is Ph+.
- Relapsed/ Refractory ALL
- 60-70% of ALL patients relapse
- If Ph+, add dastinib or nilotinib
- High relapse rate increases potential need for ponatinib
- Chronic Myelogenous Leukemia
- Incidence and Deaths (2009): 5,050 and 470
- Median age at Dx: 67 years of age (Most studies report 45-55 years)
- Male: Female = 1.5:1
- 95-100% of patients have BCR-ABL fusion protein
- Treatment Responses
- Hematologic response: normalization of peripheral blood counts
- Cytogenetic response: % of cells positive for Ph in bone marrow
- Complete- elimination of Ph
- Major- <35% Ph+ cells
- Molecular response: most sensitive; uses PCR for quantitative number of bcr-abl transcripts
- Nicolini FE et al. Epidemiologic study on survival of chronic myeloid leukemia and Ph acute lymphoblastic leukemia patients with BCR-ABLT315I mutation. Blood 2009; 114: 5271-5278.
- Median age at T315I mutation detection: 54 years
- Median time (months) between TKI treatment initiation and T315I mutation detection: 29.2(CP-CML), 15.4 (AP-CML), 5.8 (BP-CML), and 9.1 (Ph+ ALL).
- After T315I mutation detection, dasatinib and nilotinib were used in 56% of cases, hydroxyurea in 39%, imatinib in 35%, cytarabine in 26%.
- Median OS from T315I mutation detection: 22.4, 28.4, 4.0, and 4.9 months for CP-CML, AP-CML , BP-CML, and Ph ALL patients, respectively
- Median PFS from T315I mutation detection: 11.5, 22.2, 1.8, and 2.5 months for CP-CML, AP-CML , BP-CML, and Ph ALL patients, respectively
ASH 2011
Initial Findings from the PACE Trial: A Pivotal Phase 2 Study of Ponatinib in Patients with CML and Ph+ ALL Resistant or Intolerant to Dasatinib or Nilotinib, or with the T315I Mutation
- Primary Objective: Efficacy (Endpoints: major cytogenetic response for chronic phase CML or major hematologic response for accelerated phase CML, blast phase CML, and Ph+ ALL).
- Secondary Objective: Clinical and molecular responses; molecular genetic status of patients; safety
- Patients assigned to 1 of 6 cohorts based on disease+stage (chronic phase CML, ) and resistance status (resistant or intolerant of nilotinib and dastinib or T315I mutation).
- About 30% patients in chronic (64/207) or accelerated (19/60) phase CML cohorts with T315I mutation
- 46 of 48 patients in blast phase and Ph+ ALL cohort had T315I mutation
- F317L was also a common mutation
- 47% of patients in chronic phase CML cohort reached primary endpoint
- 67% of patients in accelerated CML and 37% of blast phase CML+ Ph+ ALL reached primary endpoint
- Responses for all cohorts were better than responses to most recent dasatinib or nilotinib therapy (25% CP-CML, 33% AP-CML, 25% BP-CML + Ph+ ALL).
- 67% (301/449) patients remained on study.
- Only 22% (21/94) in BP-CML + Ph+ ALL remain on study. Remember that these patients have the worse prognosis
- 4 on-study deaths were treatment related, but no evidence of ponatinib specific findings
ASH 2011 Abstracts
Analysis of the Potential Effect of Ponatinib on the QTc Interval in Patients with Refractory Hematologic Malignancies
ATP Dependent Efflux Transporters ABCB1 and ABCG2 are Unlikely to Impact the Efficacy, or Mediate Resistance to the Tyrosine Kinase Inhibitor, Ponatinib.
A Phase 1 Trial of Oral Ponatinib (AP24534) in Patients with Refractory Chronic Myelogenous Leukemia (CML) and Other Hematologic Malignancies: Emerging Safety and Clinical Response Findings
Analysis of the Potential Effect of Ponatinib on the QTc Interval in Patients with Refractory Hematologic Malignancies
- No effect on cardiac repolarization measured by lack of significant change in QTcF at all doses
Subset Analysis of Response to Treatment of Chronic Phase CML in a Phase 1 Study of Ponatinib in Refractory Hematologic Malignancies
- 81 patients (54% male) received ponatinib. 43 pts had CP-CML.
- Best responses: MCyR in 31/43 (72%), 27 (63%) CCyR.
- Complete Hematologic Response in 42/43 patients.
- Major molecular response in 19/43 (44%).
- The median time to MCyR was 12 (3-104) weeks.
ATP Dependent Efflux Transporters ABCB1 and ABCG2 are Unlikely to Impact the Efficacy, or Mediate Resistance to the Tyrosine Kinase Inhibitor, Ponatinib.
- Ponatinib is the least susceptible TKI as a substrate for efflux pumps. Nilotinib and dasatinib are the most susceptible.
AACR 2011
Ponatinib (AP24534), a potent pan-FGFR inhibitor with activity in multiple FGFR-driven cancer models with distinct mechanisms of activation
- In vitro and in vivo inhibition of FGFR of ponatinib versus other TKIs in clinical development
- Ponatinib was more potent than other TKIs and potent against different forms of FGFR
- Inhibition levels may be achieved in humans
ASH 2010
A Phase 1 Trial of Oral Ponatinib (AP24534) in Patients with Refractory Chronic Myelogenous Leukemia (CML) and Other Hematologic Malignancies: Emerging Safety and Clinical Response Findings
- At concentration of 40 nM in vitro, ponatinib inhibits many mutant forms of BCR-ABL. Based on this, the dose would need to be at least 30 mg
- Primary objective: Maximum tolerated dose or recommended dose
- Secondary objectives: safety; anti-tumor efficacy; pK/PD; pharmacogenomics
- Intra-patient dose escalation using capsules or tablets
- Patients with any stage CML (60 of 74 patients), AML, ALL, MDS, MM, or CLL
- 60 patients were Ph+
- 95% resistant to at least 2 TKIs
- Prior Treatment with imatinib (97%), dasatinib (90%), nilotinib (57%), dasatinib + nilotinib (52%)
- 28% had T315I mutant at entry; 11% with F317L mutation
- Hematologic dyscrasias most common Grade 3 AEs. Expected based on mechanism of ponatinib
- Pancreatic DLTs at 60 mg
- CP-CML: 66% MCyR, 53% CCyR, 42% MMR
- CP-CML with T315I: 100% MCyR, 89% CCyR, 78% MMR
Summary
- Ponatinib a "3rd Generation" TKI has shown great promise in terms of efficacy and safety for the treatment of CML and Ph+ ALL
- Due to long-term therapy and high rate of resistance of ALL and CML patients, ponatinib will easily find a place in therapy.
- Activity against T315I provides a solution for an unmet clinical need
- Ponatinib is the most advanced TKI in clinical development that is active against the T315I mutation
- It is encouraging that ponatinib is not likely to be a substrate for efflux pumps
- Superior results of nilotinib and dasatinib compared to imatinib in newly diagnosed patients may allow ponatinib to play a greater role in patient therapy
- It would not be surprising if ponatinib were to become first line agent for CML in the future; however, barriers would be potentially lower price of imatinib and substantially more data on safety and efficacy of imatinib
- Activity versus other receptors (FGFR and VEGFR) may lead to indications for solid tumors
- Long term efficacy and safety data still need to be collected and analyzed
- Ariad Pharmaceuticals has become an investor favorite and should continue to see great growth due to ridaforolimus and especially due to ponatinib
- Ariad is up 129.8% YTD and looks to be in the prime spot to see accelerated growth. It is possible that Ariad's 2011 year is Amgen's 1998.
Sources (not listed in-text)
Presentations of clinical data are available from Ariad Pharmaceutical's website.
CML Guideline available from National Comprehensive Cancer Network (NCCN)
O'Hare T et al. Clin. Cancer Res. 2011; 17: 212-221.
Gruber FX et al. Leukemia advance online publication, 5 August 2011; doi:10.1038/leu.2011.187